According to the latest numbers released by the Centers for Disease Control and Prevention, the share of the U.S. population that has been fully vaccinated against COVID-19 has reached 65.5 percent, and about 43 percent (140 million) of Americans have had the novel coronavirus. New research suggests that adults over the age of 50 infected with the novel coronavirus are more likely to develop shingles within six months of their diagnosis.
As reported by AARP Health, a new study published in the journal Open Forum Infectious Diseases also found that the risk of having shingles rose 21 percent for older adults hospitalized with COVID-19.
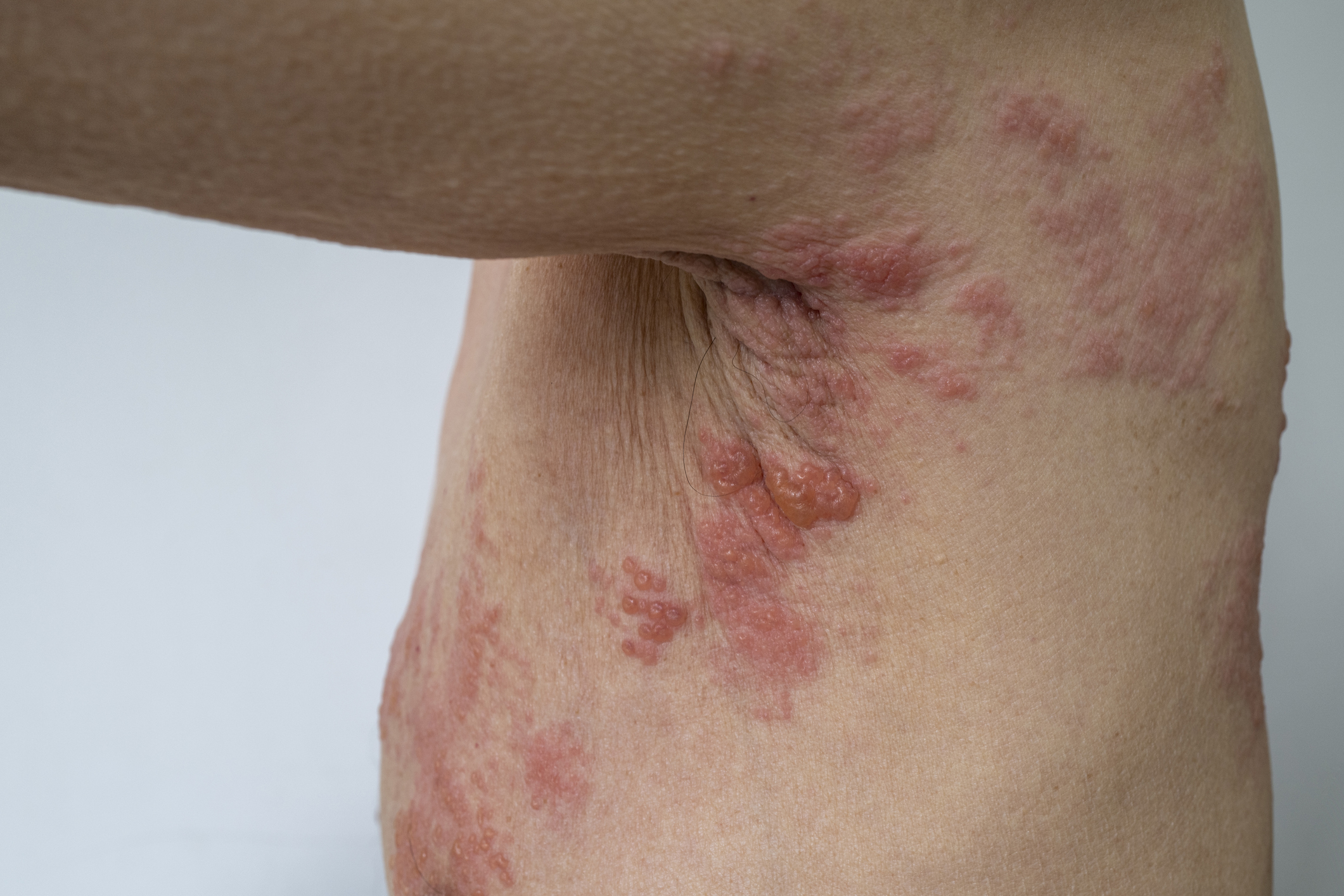
Shingles is a painful, blistering rash that is caused by the same virus (varicella-zoster) that causes chickenpox. For adults who contracted chickenpox as children, the virus can lay dormant in the body for years or even decades but can be reactivated later in life as shingles. Stress or a weakened immune system can trigger an outbreak.
Adults over the age of 50 are already at increased risk for a shingles outbreak, and since the onset of the COVID-19 pandemic, doctors have seen a significant jump in the number of shingles cases among older adults. Stress, anxiety, and depression associated with the pandemic, as well as lowered immune function from COVID-19 infection are linked with the uptick in the number of cases of shingles.
It is estimated that 1 in 3 Americans will develop shingles in their lifetime, most often over the age of 50. The lingering rash can be quite painful and can lead to serious complications if the rash spreads to the eyes or ears. The study highlights the importance for adults over the age of 50 to receive their shingles vaccine – two doses of the Shingrix vaccine have been found to be 97 percent effective in preventing shingles in people in their 50s and 60s and 91 percent successful for adults over the age of 70. The vaccine is also associated with a lower incidence of shingles-related strokes among older adults.




Add Your Voice
0 Comments
Join the Discussion